PTSD Therapy in Dubai: Key Insights and Treatment Approach
PTSD therapy in Dubai involves a structured, phased approach that helps individuals process unresolved trauma safely. Evidence-based treatments such as EMDR, DBR, and IFS work at different levels of the mind and body, supporting recovery by addressing both nervous system responses and emotional patterns.
Key Insights — PTSD Therapy in Dubai
- PTSD develops from unresolved trauma
It occurs when overwhelming experiences are not fully processed and continue to affect the mind and body. - Symptoms reflect ongoing threat response
These may include intrusive memories, flashbacks, nightmares, avoidance, and negative beliefs about the self. - PTSD therapy follows a phased approach
Treatment typically progresses through:- Safety and stabilisation
- Trauma reprocessing
- Integration
- Evidence-based therapies are central
Approaches such as EMDR and trauma-focused CBT are widely recommended in international guidelines. - Processing trauma does not always require retelling
Therapies like EMDR and DBR can work without detailed verbal disclosure, which may feel safer for many individuals. - No single therapy fits everyone
Different approaches work at different levels:- EMDR → memory processing
- DBR → early shock and orienting responses
- IFS → internal protective and wounded parts
- Integration-based therapy is often most effective
Combining approaches allows treatment to address both:- Nervous system survival responses
- Negative self-beliefs and emotional patterns
What Is Post-Traumatic Stress Disorder (PTSD)?
Post-Traumatic Stress Disorder (PTSD) is a psychiatric condition that may develop after experiencing or witnessing a traumatic event, or a series of traumatic events.
These experiences are often perceived as emotionally or physically harmful, or life-threatening. Examples include abuse (physical, sexual, or emotional), serious accidents, medical illness, natural disasters, war or combat exposure, and interpersonal violence.
However, not everyone who experiences trauma develops PTSD.
Core Symptom Patterns of PTSD
PTSD is typically described as a cluster of symptoms that reflect how the mind and body continue to respond to past overwhelming experiences.
Intrusive experiences
PTSD often involves repeated, unwanted re-experiencing of the trauma.
- Distressing memories or images may return again and again
- Thoughts may become repetitive or ruminative
- Flashbacks can occur, where brief “snippets” of the experience feel as if they are happening in the present
At times, these experiences can trigger dissociative states, where the mind automatically tries to reduce distress by creating a sense of distance, numbness, or disconnection.
LEARN MORE: WHAT IS DISSOCIATION?
Avoidance
Alongside intrusion, there is often an effort to avoid reminders of the trauma.
- Avoiding thoughts, feelings, or conversations
- Avoiding places, people, or situations that feel connected
This creates a cycle:
Intrusion brings distress → avoidance reduces it temporarily → the experience remains unprocessed → intrusion returns
Negative changes in thinking and mood
Over time, trauma can shape how a person relates to themselves and others.
- Persistent fear, guilt, or shame
- Self-critical thoughts or negative beliefs
- Loss of interest or emotional numbness
- Feeling disconnected from others or from oneself
Hyperarousal and reactivity
The nervous system may remain in a state of heightened alertness.
- Feeling constantly “on edge”
- Easily startled or sensitive to noise or movement
- Irritability or difficulty regulating emotions
- Difficulty relaxing or feeling safe
How Different Therapies Understand PTSD
Different therapeutic approaches understand PTSD in different ways. Each offers a lens into how trauma is held, experienced, and healed.
Somatic & Neuroscience-Informed Therapies (DBR, Somatic Experiencing)
From a somatic perspective, PTSD is understood as unresolved survival responses held in the body.
At the time of threat, natural processes such as
- Orienting
- Shock response
- Defensive actions (fight, flight, freeze)
may be interrupted or not completed.
As a result, the nervous system can remain in states of
- Hyperactivation (alert, anxious)
- Shutdown (numb, disconnected)
- Or alternate between hyperactivation and shutdown
These unresolved patterns continue to shape how the brain scans for danger, influencing thoughts, emotions, and behavior.
LEARN MORE ABOUT DEEP BRAIN REORIENTING THERAPY HERE.
Cognitive Behavioural Therapy (CBT)

CBT understands PTSD as a pattern of unhelpful thoughts and learned associations following trauma.
- The mind links certain cues to danger
- Thoughts such as “I am not safe” become dominant
- Avoidance reinforces fear over time
Treatment focuses on:
- Identifying and reframing thoughts
- Gradual exposure to reduce fear responses
- Building coping strategies
EMDR Therapy (Eye Movement Desensitisation and Reprocessing)

EMDR views PTSD as memories that are not fully processed and remain “stuck” in the nervous system.
These memories:
- Retain their original emotional intensity
- Are triggered in the present as if the event is still happening
EMDR helps the brain.
- Reprocess these memories
- Reduce emotional intensity
- Integrate them into a more adaptive narrative
LEARN MORE ABOUT EMDR THERAPY FOR PTSD HERE.
Internal Family Systems (IFS) Therapy

IFS understands PTSD as the result of parts of the self carrying burdens from overwhelming experiences.
- Exiled parts hold pain, fear, or shame
- Protective parts develop to manage or avoid this pain
- These protective patterns can shape behaviour, relationships, and self-perception
Healing involves:
- Building a relationship with these parts
- Releasing burdens
- Restoring balance within the system
LEARN MORE ABOUT INTERNAL FAMILY SYSTEMS THERAPY HERE.
Psychodynamic & Attachment-Based Therapies

These approaches view PTSD through the lens of early relationships and unconscious processes.
- Trauma may shape internal beliefs about self and others
- Patterns of relating (e.g. avoidance, dependency, mistrust) may develop
- Past experiences influence present emotional responses
Therapy focuses on:
- Understanding patterns over time
- Exploring relational dynamics
- Creating new experiences of safety and connection
Neurobiological Perspective
From a brain-based perspective, PTSD involves changes in how different systems function:
- The amygdala becomes more sensitive to threat
- The prefrontal cortex (thinking brain) has reduced regulatory control
- The hippocampus (memory processing) may struggle to contextualise experiences
This can lead to:
- Hypervigilance
- Intrusive memories
- Difficulty feeling safe
A Unified Understanding
Although these models differ, they point toward a shared understanding:
- Trauma is not fully processed
- The nervous system remains organised around past threat
- The present is experienced through the lens of the past
How do PTSD Therapies work?
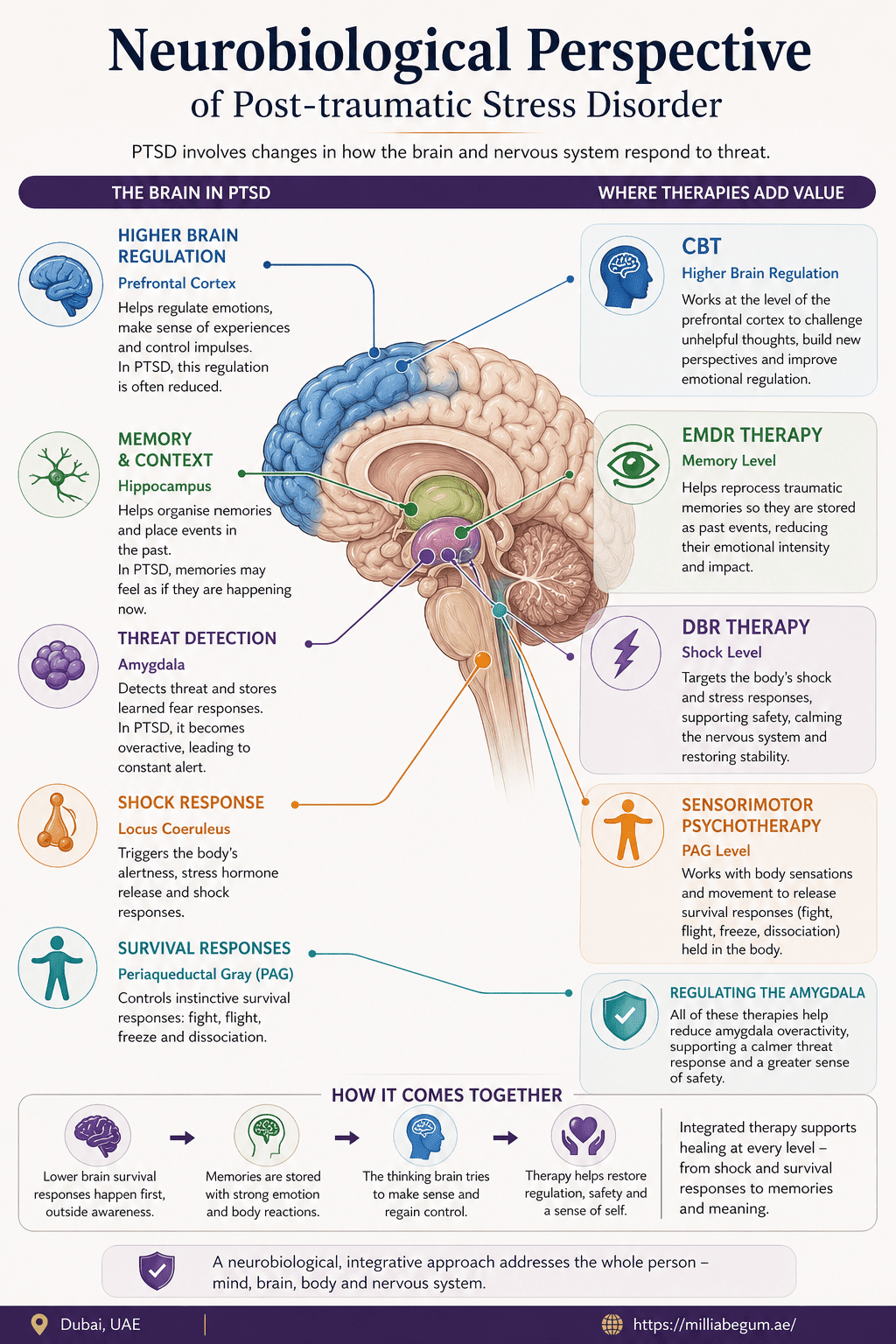
Neurobiological Perspective of PTSD and Therapy
PTSD involves changes across multiple levels of the brain and nervous system. Different therapies engage different parts of this system.
Trauma is not held in one part of the brain. Effective therapy works across levels—from early survival responses to memory to meaning-making.
CBT works at the level of higher brain regulation (prefrontal cortex), supporting thinking, perspective, and emotional control.
EMDR primarily targets memory processing networks, helping traumatic experiences to be integrated and stored as past events.
DBR therapy works with early orienting and shock responses in the midbrain before conscious emotional processing.
Sensorimotor psychotherapy works with body-based survival responses, including fight, flight, freeze, and dissociation patterns.
Across therapies, there is a shared effect of reducing overactivation of the amygdala and restoring a sense of safety.
Do PTSD symptoms affect quality of Life?
PTSD impacts not only mental health but also relationships, work, family life, and overall well-being. Many people report reduced life satisfaction, difficulties in social and occupational functioning, and challenges in maintaining daily stability.
Research Highlight: Dr. Millia Begum co-authored a study in the Journal of Mental Health showing that people with PTSD report significantly lower life satisfaction compared to those without PTSD. The findings highlight the importance of trauma-focused therapies in restoring well-being.
Real Questions People Ask About PTSD
These are some of the most common questions people ask when trying to understand PTSD, complex trauma, and trauma therapy in Dubai.
Can PTSD appear years later?
Can grief cause PTSD?
What therapy helps when talk therapy hasn’t worked?
Is PTSD therapy confidential in Dubai?
Do I have PTSD?
What are the best therapies for PTSD?
Will I ever heal from PTSD?
Will therapy help me if I cannot talk about my trauma?
Related Trauma & Treatment Resources
Post-Traumatic Stress Disorder often overlaps with attachment wounds, complex trauma, dissociation, and grief. Explore these related pages to better understand recovery pathways and trauma-focused treatment options.
Complex PTSD
Understanding prolonged or developmental trauma and its psychological impact.
Explore Complex PTSD →Attachment Trauma
How early relational trauma shapes vulnerability to PTSD symptoms.
Read about Attachment Trauma →Dissociation
Depersonalisation, derealisation, and trauma-related dissociative responses.
Learn about Dissociation →Grief & Traumatic Grief
When loss and trauma intersect, leading to prolonged or complicated grief responses.
Explore Grief Therapy →EMDR Therapy in Dubai
An evidence-based trauma treatment for processing distressing memories.
EMDR Therapy →Deep Brain Reorienting (DBR)
Addressing early orienting shock and attachment-based trauma responses.
DBR Therapy →Internal Family Systems (IFS)
Working with protective and traumatised parts of the internal system.
IFS Therapy →Book a Consultation
Comprehensive psychiatric assessment and trauma-informed treatment planning.
Contact Dr. Millia →Consultant Psychiatrist in Dubai
Learn more about trauma-focused psychiatric services.
Visit Homepage →About Dr. Millia
Dr. Millia Begum is a trained trauma specialist with over 25 years of clinical experience in psychiatry and therapy. She trained in the UK’s NHS system and served the NHS in various senior roles.
is a trained trauma specialist with over 25 years of clinical experience in psychiatry and therapy. She trained in the UK’s NHS system and served the NHS in various senior roles.
She is a former EMDR Europe Approved Consultant, EMDR researcher, and board member of the EMDR Association UK. She is now a member of the EMDR International Association (EMDRIA).
Dr. Millia is a Certified Internal Family Systems (IFS) Therapist, bringing a compassionate, parts-informed approach to her work with clients in Dubai.
Contact Dr. Millia
If you would like to book a consultation or learn more about services, please get in touch:
- Clinic: First Psychiatry Clinic
- Address: 975 Al Wasl Road, Dubai, UAE
- Phone: +971 55 355 7855
- Email: info@milliabegum.ae
- Website: milliabegum.ae
